Gynecologic causes of acute pelvic pain:
Functional and hemorrhagic ovarian cysts:
Follicular cyst:
During the first half of the menstrual cycle, many ovarain follicles enlarge under the effect of FSH & eventually one or more turn into a dominant follicle which usually measures about 18 -25 mm. Ovulation is then triggered by the surge of LH and the dominant follicle converts into corpus luteum. If a dominant follicle fails to expel an oocyte, it may further enlarge in size forming a follicular cyst which appears as thin-walled, unilocular, anechoic & avascular lesion with posterior acoustic enhancement. It usually ranges in size from 3-8 cm.
Corpus luteum cyst:
The corpus luteum forms after ovulation and slowly regresses throughout the remainder of the menstrual cycle. If it fails to involute, a corpus luteal cyst may form & demonstrate a thick, irregular wall on ultrasound with increased peripheral vascularity on Doppler scan.
Hemorrhagic ovarian cyst:
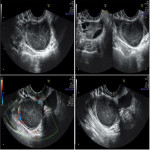
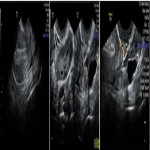
The sonographic appearance of hemorrhagic ovarian cysts is variable. One of the typical sonographic appearances of a hemorrhagic cyst is that of a complex mass with internal echoes and the “lace-like” or “spider-web” pattern of internal fibrin reticulation which are avascular on color Doppler imaging. A blood clot can appear as a solid triangular or curvilinear echogenic structure within the cyst. Fluid-debris levels can develop as the clot liquefies. When a hemorrhagic cyst ruptures, echogenic free fluid (hemoperitoneum) will be visible in the pelvis (figure 1).
Endometrioma:
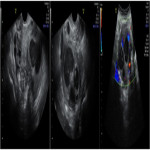
Endometriosis is the presence of endometrial tissue outside its normal location in the uterus. Ectopic endometrial tissue is most commonly found in the ovaries (80%), broad ligaments, fallopian tubes, and cul-de-sac. A cystic mass with homogeneous low-level internal echoes or “ground glass” appearance is a characteristic sonographic appearance of endometrioma (figure 2). However, endometriomas have variable appearances on sonography like fluid level, multilocularity and the quite typical echogenic cholesterol foci within the wall of the cyst.
Ovarian Torsion:
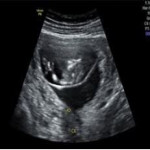
Ovarian torsion is partial or complete twist of the ovary on its vascular pedicle secondary to an existing benign adnexal mass. However it may occur in normal ovaries. The prompt diagnosis of ovarian torsion is crucial to allow conservative ovary-sparing surgical intervention. Ovarian enlargement is one of the most common sonographic features of ovarian torsion (figure 3). Other sonographic findings of ovarian torsion are: non ovulatory follicles measuring up to 2.5 cm at the periphery of the enlarged ovary, abnormal location of the ovary and free fluid around the affected ovary or in the Douglas pouch. Fluid-debris levels within the peripheral cysts is pathognomonic of torsion. The follicular ring sign (figure 4) is also pathognomonic for the early diagnosis of torsion. It represents a prominent (1-2 mm thick) hyperechoic margin seen concentrically around the peripherally displaced follicles of the torsed ovary, which are usually small (3‐7 mm in diameter). The whirlpool sign of the twisted vascular pedicle can be also visualized on ultrasound. Absence of blood flow on Doppler imaging helps to clinch the diagnosis of ovarian torsion. However, the persistence of vascular flow does not rule out the possibility of torsion.
Ectopic pregnancy:
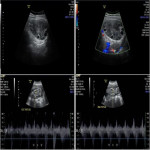
The fallopian tube is the most common location of ectopic pregnancy. Other types of ectopic pregnancy include cornual, ovarian, interstitial, scar, and rarely, cervical and intra-abdominal. Transvaginal ultrasound is the preferred method of evaluation when ectopic pregnancy is suspected. The most common finding of tubal ectopic pregnancy is the presence of an extrauterine gestational sac or complex solid mass which is separate from the ovary (figure 5) in absence of intrauterine pregnancy or presence of a pseudogestational sac. The tubal ring sign represents a hyperechoic ring surrounding an extrauterine gestational sac & is characteristic for tubal pregnancy. Doppler scan can reveal peripheral hypervascularity with high-velocity low impedance flow of the hyperechoic ring of the extrauterine gestational sac and referred to as “ring of fire” sign which is not specific for ectopic pregnancy. Visualization of an extrauterine gestational sac with a live embryo is 100% specific for an ectopic pregnancy. The presence of free pelvic fluid in a woman with a positive pregnancy test and no intrauterine pregnancy are highly suggestive of ectopic pregnancy.
Pelvic Inflammatory Disease / Tubo-ovarian Abscess:
Pelvic inflammatory disease refers to an infection of the upper reproductive tract, including endometritis, salpingitis, and oophoritis typically ascending from lower tract infection. In the early stage of the disease, sonographic findings are usually very subtle and can not be easily detected. Uterine enlargement with ill-defined soft tissue margins and fluid within the endometrial cavity are suggestive of endometritis. Distended, fluid-filled, folded, and tubular structures with tapering ends in the adnexal regions are the key findings in hydrosalpinx. Thickened hyperemic walls with thickened endosalpingeal folds (having cog-wheel appearance) in cross-section and complex luminal fluid with floating echoes are indicative of pyosalpinx. The inflamed ovary (figure 6) is usually swollen and can attain a reactive polycystic appearance with increased parenchymal vascularity on Doppler scan. Pelvic free fluid can also be seen. Tubo-ovarian abscess may form at later stages and appears as a complex, mixed solid and cystic adnexal mass.
Pregnancy-related causes of acute pelvic pain:
Placental abruption:
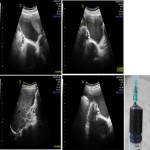
Placental abruption, is the partial or complete premature separation of a normally implanted placenta from the myometrium. It can be divided into revealed & concealed abruption. The diagnosis of placental abruption is usually clinically established based on the presence of pelvi-abdominal pain, vaginal bleeding and uterine tenderness. The most common type of intrauterine hemorrhage is subchorionic hemorrhage which usually results from abruption of the placental margin in the late first trimester (figure 7). Retroplacental hematoma is more common after 20 weeks’ gestation and preplacental (subamniotic) hematoma is the least common type. On ultrasound, intrauterine hemorhages appear as crescent-shaped areas with variable echogenicity, depending upon the age of the blood products. Acute blood appears hyperechoic to isoechoic when compared to the placenta and may be interpreted as a thick placenta and it becomes hypoechoic by 1 week from the initial event and sonolucent by 2 weeks.
Non-gynecologic causes of acute pelvic pain:
Appendicitis:
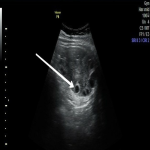
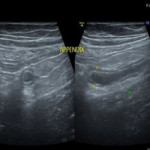
Appendicitis is the most common cause of acute right lower abdominal pain. Ultrasound is not only useful in the diagnosis of appendicitis but also useful in exclusion of other causes of pelvic pain and avoiding the unnecessary surgical management in patients with atypical clinical presentations. Inflamed appendix appears as a distended, noncompressible blind ended structure with a diameter greater than 7 mm (figure 8). Identification of an appendicolith is helpful in confirming the diagnosis. Other findings which can aid in the diagnosis of appendicitis are echogenic surrounding fat planes, reactive mesenteric lymphadenopathy and presence of reactive free fluid. Peri-appendiceal abscess usually appears as a hypoechoic fluid collection with mass effect on the surrounding structures.
Ureteric stones:
Ureteric stones in women typically causes flank pain which refers to the ipsilateral groin and vulva. They are typically diagnosed by the detection of hydronephrosis and visualization of the calculus in the ureter which appears as an echogenic structure with distal acoustic shadowing. The role of ultrasound can be limited in evaluating ureteral calculi as the ureter can be well examined only in its most proximal and distal portions. CT is more sensitive for detection of ureteral calculi.
Diverticulitis:
Diverticulitis is caused by inflammation of an outpouching of the colon. Acute diverticulitis can be identified during an ultrasound evaluation of a premenopausal woman presenting with acute pelvic pain. However, CT is considered the “gold standard” for its diagnosis. A non-compressible outpouching of a bowel loop showing thickened and hypoechoic wall associated with adjacent bowel wall edema & thickening, and edematous hyperechoic surrounding mesenteric fat are the main sonographic findings seen in diverticulitis. Associated localized tenderness can be noted on gentle compression with the ultrasound transducer. Perforation, fistula and abscess formation are the most common complications of diverticulitis. Abscess usually appears as a hypoechoic collection on ultrasonography.
Other potential non-gynecologic causes:
Mesenteric adenitis, bowel obstruction, inflammatory bowel disease, and metastatic disease are also considered in the differential diagnosis of acute pelvic pain in reproductive women and should be ruled out during the examination of patients fitting the criteria.