5 Differences Between Canker Sores and Cold Sores
Key takeaways:
Cold sore is another name for oral herpes. The herpes simplex virus (HSV-1) causes cold sores.
Canker sores, or aphthous ulcers, have many different causes. Their effects can range from mild to quite serious.
Both canker sores and cold sores tend to show up again and again over time. But you can usually tell them apart based on when and how they appear.
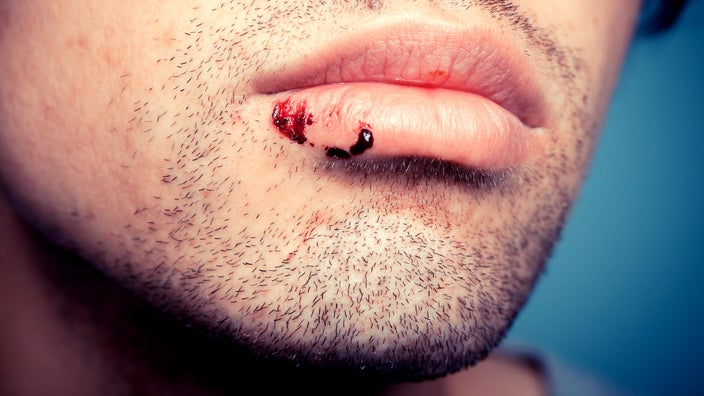
A mouth sore can make it hard to eat, drink, brush your teeth, and sometimes even talk. They can also be embarrassing, especially when they show up on the outside of your lips. But are they really a serious problem?
Most mouth sores are either cold sores or canker sores. While these names might sound pretty similar, the distinction between them is important. Keep reading to learn the difference between cold sores and canker sores, and what to do if you think you have one.
1. Oral herpes causes cold sores but not canker sores
Understanding the difference between canker sores and cold sores begins with knowing a bit about what causes them.
The herpes simplex virus (oral herpes) causes cold sores
This might be alarming, after all, genital herpes is a well-known sexually transmitted disease (STD). But oral herpes is different from genital herpes, and having a cold sore doesn’t mean you have an STD.
Cold sores and genital herpes are caused by different strains of the herpes simplex virus (HSV) — HSV-1 and HSV-2. Both HSV-1 or HSV-2 can cause genital herpes, but HSV-1 almost always causes cold sores around the mouth. And HSV-1 is common: Research suggests that over half of U.S. adults have been infected with it.
Canker sores have many causes
Unlike cold sores, canker sores have a long list of possible causes, including:
Other viral infections: like coxsackie virus (which causes hand, foot, and mouth disease), cytomegalovirus (CMV), or the human immunodeficiency virus (HIV)
Injury or trauma: like after biting the inside of your cheek; or for babies, during teething or after a toy-related injury
Autoimmune disorders: such as celiac disease or systemic lupus erythematosus
Nutritional deficiencies: like low levels of iron, folate, vitamin C, or vitamin B12
Bacterial or fungal infections: such as syphilis, tuberculosis, or Valley fever
Hormonal changes: such as those related to your menstrual cycle
With so many different causes, it’s likely that everyone gets canker sores at some point — and most of the time we never know what causes them. A single canker sore, or a single group of canker sores, that comes and goes within 1 to 2 weeks usually isn’t a big deal.
2. Cold sores and canker sores look different and show up in different places
You can often tell the difference between cold sores and canker sores based on what they look like and where they show up.
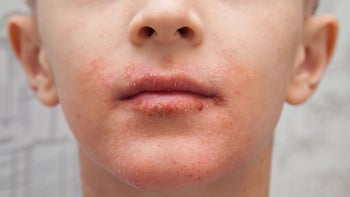
A cold sore (oral herpes) is usually a large blister or crust on the lip
A typical cold sore starts as a blister on the pink outside surface of your lip. Over a couple of days the blister grows larger, breaks, and turns into an open sore. Then it crusts over and heals. The whole process takes a couple of weeks.
But there’s one important note: If you’ve never had HSV-1, you might have a different experience when you catch it for the first time. A new infection with HSV-1 can sometimes cause herpes gingivostomatitis. This is a condition that comes with a fever and dozens of painful sores inside the mouth, across the tongue, and on the gums.
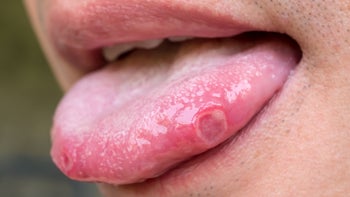
Canker sores can happen inside the mouth or nose
Canker sores aren’t as predictable as cold sores. They can show up anywhere on your mucous membranes — that is, anywhere on the moist, pink skin inside your mouth or nose.
Canker sores often start out as a single small ulcer, although this depends on the cause. Over a few hours or days they can grow larger and more painful, and more ulcers can appear nearby.
3. Cold sores and canker sores follow different patterns over time
Another important piece in understanding mouth sores is when they occur.
Cold sores tend to come back during times of stress.
If you’re a person who gets cold sores, you’ll find they pop up during times of stress — and not just psychological stress. Anything that stresses your body, from illness to ultraviolet (UV) sunlight exposure, can trigger a cold sore.
This happens because HSV never goes away completely. Instead, it hides deep inside your nerve cells, where it can stay for years without causing problems. It reemerges when you’re most vulnerable.
Many canker sores are isolated, but they can return in a pattern
Anyone can get a one-off canker sore or even a group of canker sores that appears and then fades over time. This is the case for most people.
But some people tend to get recurring canker sores, over and over again. This is typical with certain medical conditions, like:
Cyclic neutropenia
Periodic Fever, Aphthous Stomatitis, Pharyngitis, Adenitis syndrome (PFAPA)
In these cases, canker sores also tend to come on during times of stress. But unlike cold sores, recurring canker sores often come with other symptoms, like fevers, joint pain, or rashes.
If you tend to get mouth sores over and over again, it’s worth talking to a healthcare provider. Sometimes blood work or other tests are needed to figure out what’s going on.
4. Cold sores (oral herpes) are contagious — canker sores are not
When you have a mouth sore, the last thing you want to do is spread it to others — especially if it can cause problems.
Cold sores are very contagious, and HSV can be dangerous
HSV, the virus that causes cold sores, can spread between people very easily. It spreads fastest when you have an open sore — that is, after the blister has broken open and before a crust has formed over it. But it can spread any time you have symptoms.
Although HSV is not usually dangerous for healthy adults, it can be a major problem for some people. In particular, HSV can cause life-threatening infections in:
Newborns
Older adults
People who are immunocompromised or who have suppressed immune systems
Anyone with a cold sore should stay away from vulnerable individuals, including people who are pregnant and near to term.
Canker sores can be painful, but usually they are not dangerous
Most of the time canker sores aren’t contagious. Even when they are linked to an infection, they don’t tend to be a major source of germ spreading.
That isn’t to say canker sores aren’t a big deal. They can be very painful. And sometimes they can be a sign that something else is going on, especially when they keep coming back.
5. The treatment for cold sores and canker sores is completely different
Although both types of mouth sores might call for pain control, the way you’ll want to handle them is quite different.
You can treat cold sores with antiviral medication if you catch them quickly
People who get cold sores often know when they’re about to get one. That’s because they experience a tingling feeling on their lip right before the cold sore appears.
That warning sign is helpful, because if you start treatment quickly, you can stop the cold sore in its tracks. In fact, if you start the medication really quickly, you might even be able to keep the cold sore from fully appearing.
Docosanol (Abreva) is an over-the-counter (OTC) antiviral cream that can be helpful against HSV. It works best when you start it at the first hint of a cold sore. To be effective, you need to use it five times per day.
Prescription oral antiviral medications are very effective against HSV. Again, they work best if you start treatment right away. You take these by mouth several times per day:
Acyclovir (Zovirax)
Valacyclovir (Valtrex)
If you are someone who gets frequent cold sores, you’ll want to talk with your healthcare provider about having a prescription for an oral antiviral ready to go quickly in case your symptoms return. Another possible option is to take antivirals every day to prevent cold sores.
There’s no specific treatment for canker sores — but there are things you can do to help
Canker sores are more difficult to treat than cold sores. Since the cause of canker sores is often a mystery, their treatment often has to do with fighting the pain until they go away on their own.
OTC options for treating the pain of canker sores include:
Acetaminophen (Tylenol), ibuprofen (Advil or Motrin), or naproxen (Aleve)
Oral analgesic gel with benzocaine (Anbesol, Orajel, or Zilactin-B)
Oral rinse with hydrogen peroxide (Orajel or Peroxyl)
Natural remedies for the pain of canker sores include:
Alum (potassium sulfate) powder, used as a paste
Saltwater rinses
Baking soda rinses
Honey, applied with a swab several times per day
Milk of magnesia, applied with a swab several times per day
In severe situations, prescription options, such as steroids, can also help with the pain of canker sores.
The bottom line
Both canker sores and cold sores are common, and they can be easy to confuse. But understanding the difference between them is important. The cause of cold sores is an oral herpes virus (HSV-1), and it can spread easily to others. But you can treat a cold sore with medication if you catch it quickly. On the other hand, canker sores are usually more of a nuisance and don’t have a specific treatment.
References
Aslanova, M., et al. (2021). Herpetic gingivostomatitis. StatPearls.
Chi, C. C., et al. (2015). Interventions for prevention of herpes simplex labialis (cold sores on the lips). Cochrane Database of Systematic Reviews.
Edgar, N. R., et al. (2017). Recurrent aphthous stomatitis: A review. Journal of Clinical and Aesthetic Dermatology.
Rafieian, N., et al. (2016). Efficacy of alum for treatment of recurrent aphthous stomatitis. Caspian Journal of Internal Medicine.
Xu, F., et al. (2006). Trends in herpes simplex virus type 1 and type 2 seroprevalence in the United States. Journal of the American Medical Association.
Yan, C., et al. (2020). Disturbed yin-yang balance: Stress increases the susceptibility to primary and recurrent infections of herpes simplex virus type 1. Acta Pharmaceutica Sinica.